Sustained emotional distress within intimate relationships is a measurable stressor with documented physiological consequences — consequences that compound silently in individuals whose professional performance demands sustained cognitive output and physiological resilience. For executives and founders operating at high output, chronic relational pain elevates circulating cortisol, disrupts HPA axis regulation, and accelerates telomere attrition — a direct marker of biological age. When love is hurting, the damage is not confined to mood or motivation. It registers in the body's stress architecture, undermining the very systems — immune function, sleep quality, executive cognition — that high performers depend on most.
The Physiology of Relational Pain

Emotional pain activates many of the same neural pathways as physical pain. Functional MRI research shows that social rejection and interpersonal loss engage the anterior cingulate cortex and anterior insula. These regions are central to processing physical discomfort. So when love is hurting, the brain does not treat that experience as metaphorical. It registers it as threat.
That threat signal then triggers the same stress cascade designed for acute physical danger. For high-performing professionals, the problem is not a single activation of this system. It is the repetition. A relationship generating sustained low-grade distress — unresolved conflict, emotional withdrawal, chronic disconnection — keeps the HPA axis in a state of partial activation.
As a result, the body runs a background stress program it was never designed to sustain. Energy that would otherwise support tissue repair, immune function, and cognitive restoration gets redirected toward threat management. This is not a psychological inconvenience. It is a measurable metabolic burden.
Cortisol, Chronicity, and the HPA Axis
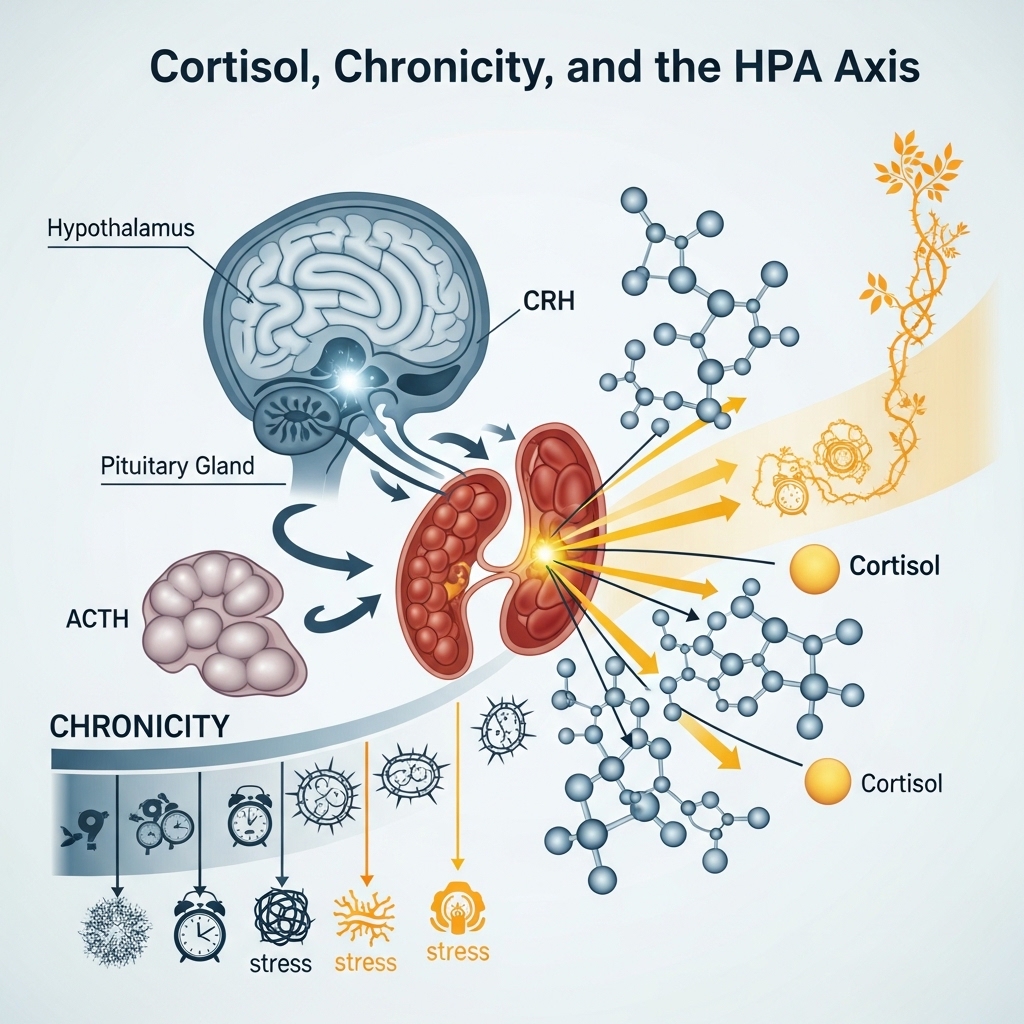
The stress response is adaptive in short durations. Cortisol mobilises glucose, sharpens attention, and prepares the body for action. However, the system was not designed for sustained activation without resolution.
Chronic relational distress functions as a non-resolving stressor. Unlike a deadline or a difficult negotiation — both of which have clear end points — a troubled intimate relationship generates persistent low-intensity threat signals. Consequently, NIH-referenced psychoneuroimmunology research documents that sustained psychosocial stressors produce dysregulated cortisol rhythms. These flatten the daily cortisol curve essential for healthy metabolic and immune function.
A flattened cortisol curve carries real clinical weight. Specifically, it links to increased inflammatory activity, disrupted glucose regulation, and impaired cognitive performance — particularly in working memory and executive function. For professionals whose output depends on sustained mental precision, this is a direct and measurable performance liability.
Inflammatory Markers and the Relational Environment

The connection between relationship quality and systemic inflammation is well documented. Research from the Institute for Behavioral Medicine Research at The Ohio State University shows that couples engaging in hostile conflict display measurable elevations in pro-inflammatory markers — including interleukin-6 (IL-6) and tumor necrosis factor-alpha (TNF-α). These elevations appear in blood samples taken within hours of conflict exposure.
Systemic inflammation drives faster biological aging. Specifically, it underpins arterial disease, metabolic problems, neurodegeneration, and a range of cancers. Moreover, inflammaging — the chronic low-grade inflammatory state that builds with age — worsens with sustained psychosocial stress. A relational environment defined by chronic distress therefore accelerates this process directly.
For professionals tracking longevity markers — CRP, IL-6, or oxidative stress indices — the relational environment belongs in that analysis. Optimising sleep, training, and nutrition while operating within a chronically distressing relationship means managing downstream symptoms. The upstream stressor remains unaddressed.
Cardiovascular Consequences of Chronic Emotional Stress

The cardiovascular system responds directly to relationship quality. The Framingham Heart Study and subsequent longitudinal research establish that psychosocial stressors — including marital stress and social isolation — function as independent risk factors for cardiovascular events. The mechanisms include autonomic disruption, elevated resting heart rate, increased arterial stiffness, and impaired heart rate variability (HRV).
HRV is a metric many high-performing professionals monitor as a proxy for recovery capacity. Low HRV connects not only to overtraining and poor sleep, but also to chronic psychological stress. Furthermore, a persistently distressed relational environment suppresses parasympathetic activity — the branch of the autonomic nervous system responsible for recovery and regulated cardiac output. Over time, this produces measurable HRV decline.
The American Heart Association now recognises psychosocial health as a component of cardiovascular risk assessment. This places chronic relational pain within the domain of cardiovascular medicine. Professionals who track cardiovascular age or arterial health should therefore treat relationship quality as a variable equal in standing to diet, exercise, and sleep.
Sleep Architecture Disruption

Sleep is the primary recovery mechanism available to the human body. During deep slow-wave sleep, the body releases growth hormone, initiates cellular repair, clears neurotoxic waste, and consolidates immune memory. Any stressor that degrades this process carries significant consequences for both performance and longevity.
Chronic relational distress reliably disrupts sleep. Elevated night-time cortisol — a product of sustained HPA axis activation — impairs sleep onset, reduces slow-wave sleep, and increases early waking. In addition, behavioural sleep medicine research shows that individuals in high-conflict or emotionally draining relationships report significantly poorer sleep quality. Polysomnographic data confirm measurable differences in their sleep structure.
For a high-performing professional, degraded sleep compounds with precision. The consequences include reduced reaction time, impaired emotional control, increased appetite for high-reward food and stimulants, weakened immune function, and faster cellular aging. When love is hurting and sleep suffers, every recovery system takes a measurable hit.
Cognitive Performance and Executive Function

The prefrontal cortex — the neural hub of strategic reasoning, impulse control, and long-term planning — shows acute sensitivity to cortisol. Sustained cortisol elevation causes structural changes in prefrontal neurons, reduces synaptic flexibility, and impairs working memory. Moreover, prolonged exposure produces changes now visible on neuroimaging.
The Harvard Study of Adult Development — one of the longest-running studies on adult wellbeing — consistently finds that intimate relationship quality ranks among the strongest predictors of sustained cognitive function in later life. This mechanism is not purely psychological. It runs through HPA axis regulation, inflammatory signalling, and sleep quality — the same pathways that govern the rate of cognitive aging.
For executives and founders, the cognitive costs of chronic relational distress appear long before any clinical threshold. Reduced clarity in decisions, diminished creative thinking, shorter attention endurance, and increased emotional reactivity under pressure all follow. Furthermore, these consequences register in boardrooms and leadership settings — often without any clear link back to their relational source.
Attachment Dysregulation and Autonomic Load
Adult attachment patterns — relational templates shaped by early life and refined through intimate partnerships — directly affect autonomic nervous system function. Individuals with insecure attachment orientations show characteristic autonomic disruption in relational contexts. Specifically, anxiously attached individuals display elevated sympathetic arousal, while avoidantly attached individuals show suppressed parasympathetic function.
These are not fixed personality traits. Instead, they are dynamic physiological states that shift with the relational environment. A relationship that repeatedly activates attachment threat — through inconsistency, emotional absence, or ongoing conflict — holds the autonomic system in a dysregulated state. The body does not distinguish between a predator and an emotionally unavailable partner when both register as threat.
The clinical implication is direct. This form of autonomic disruption links to elevated inflammatory markers, impaired HRV, disrupted cortisol rhythms, and faster vascular aging. As a result, attachment science now has clear applications in longevity medicine and high-performance physiology.
READ ALSO: Relationship Stages: Navigate Connection With Ease
Telomere Attrition and Biological Age
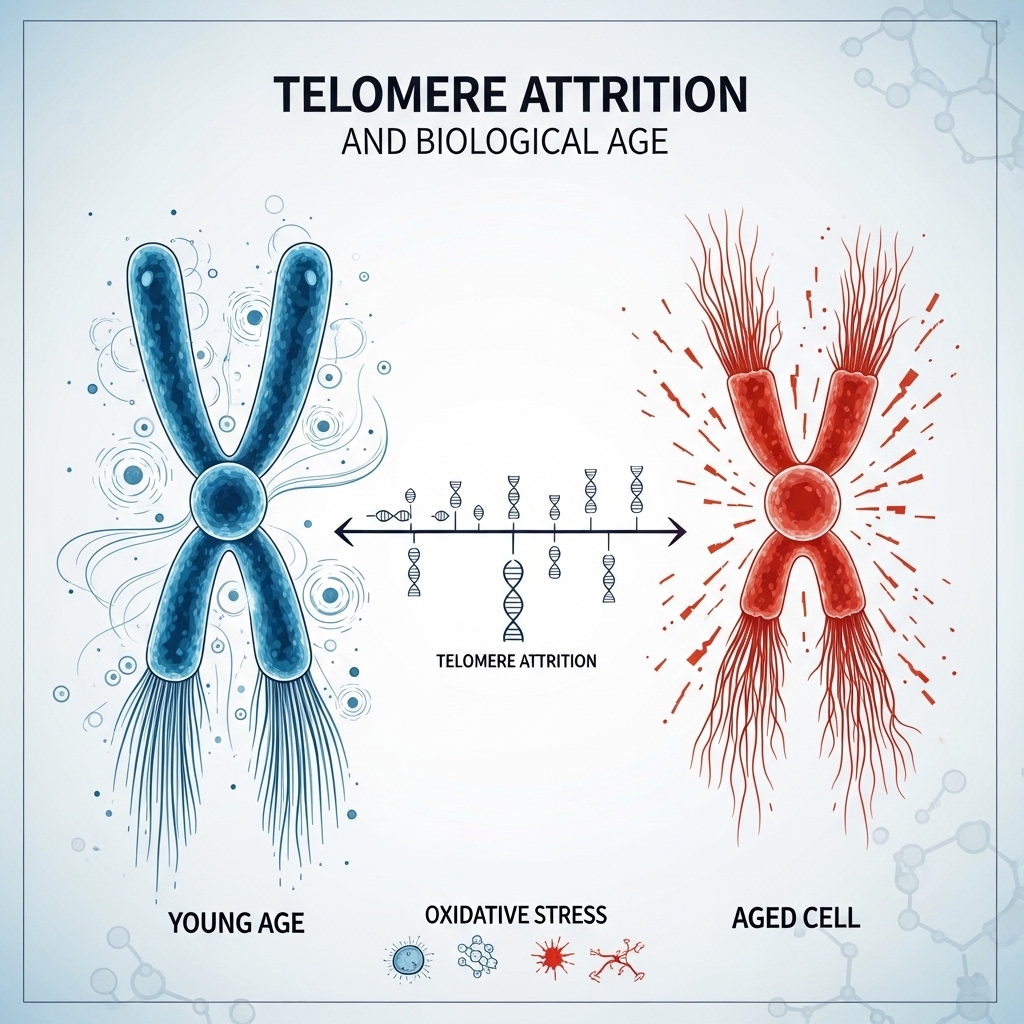
Telomeres — the protective caps at the end of chromosomal DNA — shorten with each cell division and with cumulative oxidative stress. Telomere length serves as one of the most widely used molecular markers of biological age. Accelerated shortening links to earlier onset of age-related disease and reduced lifespan.
Research published in journals including Psychoneuroendocrinology documents that chronic psychological stress — particularly in interpersonal contexts — links to significantly shorter telomere length. The proposed mechanisms include cortisol-driven oxidative stress, elevated inflammatory markers, and mitochondrial dysfunction. Sustained relational distress worsens all three.
For professionals who track biological age through validated tools — epigenetic clock testing, telomere assays, or composite biomarker panels — the relational environment directly influences the output. When love is hurting over an extended period, the gap between chronological age and cellular age is likely to widen.
The Suppression Dynamic in High Performers
High-performing professionals often excel at emotional suppression. This is not a pathological defence — it is a practised operational strategy. Bracketing emotional content to maintain executive function under pressure is a genuine skill in high-stakes environments. As a chronic relational strategy, however, suppression carries a distinct physiological cost.
Affective neuroscience research shows that emotional suppression increases sympathetic nervous system activation. It raises physiological arousal even when outward behaviour appears contained. Specifically, individuals who habitually suppress responses to relational pain show higher baseline cortisol, elevated inflammatory markers, and greater cardiovascular reactivity than those who process and express emotional content.
The operational logic that serves a founder in a crisis — contain the emotion, execute the decision — becomes a chronic liability in the relational domain. Sustained suppression of relational pain does not resolve the underlying stressor. Instead, it compounds the biological cost while silencing the signal that might otherwise prompt action.
READ ALSO: Relationship Symbiosis: Nurturing Balanced Partnerships
Relationship Quality as a Longevity Variable

The field of social genomics — advanced significantly through the work of Dr. Steve Cole at UCLA — demonstrates that the social environment directly influences gene expression. It modulates the activity of genes involved in inflammatory response, antiviral defence, and stress reactivity. Intimate relationship quality ranks among the most potent social variables affecting this gene expression profile.
This positions relationship quality not as a soft lifestyle factor but as a hard biological input with measurable genomic consequences. Moreover, the same analytical rigour applied to VO2 max, lipid panel management, or micronutrient status applies equally to the relational environment. A high-performing professional who treats relationship quality as peripheral to their health strategy is working with an incomplete model of their own biology.
Longitudinal data consistently places social relationship quality among the top predictors of both healthspan and lifespan. Its effect size is comparable to smoking cessation, physical activity, and dietary quality. When love is hurting, the body receives a continuous signal that degrades the biological systems sustaining performance, recovery, and longevity.
READ ALSO: Therapist Relationship: Building Trust That Works
Evidence-Based Pathways for the High-Performing Professional

The evidence reviewed here does not point to a single intervention. What it supports is the recognition that relational health belongs in the same category as sleep, cardiovascular training, and metabolic management. Professionals who identify chronic relational distress as a stressor may consider working with a clinically trained couples therapist or psychologist with expertise in attachment and conflict physiology.
Structured somatic practices — including HRV biofeedback and breathwork protocols — carry documented efficacy in reducing HPA axis dysregulation. These approaches work independently of the relational context itself, making them accessible starting points. In addition, biomarker monitoring — CRP, cortisol rhythm testing, HRV tracking, and biological age assessments where accessible — provides objective data to inform both the severity of physiological burden and the response to any intervention.
The clinical literature does not support passive tolerance of chronic relational distress as a manageable background condition. Rather, it supports active engagement with it as a health variable. Left unaddressed, it compounds against every other investment a high-performing professional makes in their longevity.
UP NEXT: Relationship Coaches: Finding Support Without Pressure
Chronic relational distress elevates cortisol, drives systemic inflammation, and accelerates telomere attrition — three of the most direct biological pathways to faster cellular aging, with sustained relational stress linked in longitudinal research to measurable increases in biological age relative to chronological age. WholeLiving's Biological Age Estimation Model incorporates this factor directly — your assessment takes under five minutes.
Ready to understand how these factors are influencing your biological age right now? [Take the Biological Age Assessment →]






